The landscape of Singapore's medical education has flourished over the years, resulting in the three local medical schools we know today: NUS Yong Loo Lin School of Medicine (NUS Medicine), National University of Singapore (NUS), Duke-NUS Medical School and Lee Kong Chian School of Medicine (LKCMedicine), Nanyang Technological University, Singapore (NTU). In appreciation of the continuing development of local medical education and the progress made, SMA News invites representatives from the three medical schools to share and reflect on their respective curricula.
Shelvi and Adj Prof Lau Tang Ching
As healthcare grows in complexity, medical education must adapt to prepare doctors for current and future demands. NUS Medicine has undertaken a comprehensive curriculum transformation aligned with Singapore's national priorities. This reform is anchored in two Ministry of Health (MOH) initiatives:
Embedding these standards ensures NUS Medicine graduates are clinically competent, person-centred and ready to contribute to the health system from day one.
The transformation is guided by clearly defined graduate outcomes that shape every aspect of the curriculum. Beyond knowledge acquisition, the school's vision cultivates a holistic professional identity through the "six roles of a well-rounded doctor". These six roles form a comprehensive definition of the modern physician, which drives the curriculum's tangible innovations. Graduates are expected to be:
- Safe and effective clinicians who exercise sound judgement and deliver person-centred care;
- Critical thinkers, scientists and scholars grounded in the social and scientific foundations of medicine;
- Kind and compassionate professionals who communicate clearly, respond sensitively to patients and act with integrity;
- Partners and team players who collaborate effectively and show leadership in clinical care, education and research;
- Dynamic learners and educators who are adaptable, committed to lifelong learning and comfortable with emerging technologies such as artificial intelligence (AI); and
-
Advocates for health improvement who positively and responsibly impact individual, community and population health.
Redesigned from the ground up
To turn this philosophy into practice, NUS Medicine has redesigned medical training through interprofessional education, greater clinical relevance and integrated technology.
A new cornerstone is the Common Curriculum for Healthcare Professional Education (CCHPE), launched in August 2023 for undergraduates in medicine, nursing, dentistry and pharmacy. Delivered over the first two years, it comprises five courses: Socio-Ecological Determinants of Health; Professional Practice 1 and 2; Data Literacy for Healthcare; and Digital Literacy for Healthcare. The CCHPE breaks down professional silos early, fostering mutual respect, shared language and a collaborative mindset essential for preventive, person-centred, team-based care aligned with the Healthier SG initiative. This is reinforced by the Longitudinal Patient Experience programme, where interdisciplinary student groups visit patients in their homes over a year, applying classroom concepts in real-world community contexts and deepening patient-centred care.
Preclinical education has shifted from traditional subject-based teaching to a clinically integrated, organ-system model. Instead of learning anatomy, physiology and pathology in isolation, students study systems such as cardiovascular and neurological, connecting normal biology to disease in a cohesive, clinically relevant context. Each year culminates in a multi-system block capstone, challenging students to apply foundational science to complex clinical problems affecting multiple systems and sharpening clinical reasoning.
Clinical training in Phases III to V has been refined to ensure consistent quality and progressive competence. EPA milestones are embedded to guide performance and assessment, and postings are standardised for clarity and consistency. The final year has been restructured into two courses. The first comprises revision postings preparing students for the Final Professional MBBS examination. The second is a revamped Student Internship Programme (SIP) that shifts away from high-stakes summative exams, emphasising workplace-based assessments and EPA-aligned tasks. SIP concludes with a multi-station objective structured clinical examination focused on practical skills essential for a first-year postgraduate doctor, aligning assessment with real-world responsibilities.
Technology and simulation are integrated throughout the curriculum to enrich learning and develop adaptable, self-directed clinicians. High-fidelity tools such as the Harvey cardiopulmonary simulator and SimMan manikins provide hands-on practice in a safe environment. Home-grown virtual reality programmes include PASS-IT for patient safety in surgery, VRAM in psychological medicine, a VR delivery suit programme and RESCUE VR for trauma training. Gamified tools make complex topics engaging. For example, HEALING teaches healthcare economics and PRESCRIBE develops safe prescribing skills. These resources mirror technologies in modern clinical practice and build comfort with digital innovation, fostering lifelong learning.
To future-proof graduates, the curriculum offers structured pathways for specialisation in data-driven discovery and research. The new Minor in Biomedical Informatics equips students to use and innovate with data and technology, improving patient outcomes, operational efficiency and research. In parallel, the Beyond Medicine programme nurtures research capability and curiosity, including a one-day research festival that connects students with research groups and shows how bedside questions can drive impactful projects. Guided opportunities encourage students to pursue inquiry that translates into improved health outcomes.
This transformation is both structural and developmental, designed to meet Singapore's evolving healthcare needs while preparing graduates to excel as clinicians, collaborators and innovators. Its success rests on strong stakeholder engagement, ongoing faculty development and rigorous evaluation to identify areas for improvement. NUS Medicine remains committed to continuous refinement, with an ambition to train the doctors of the future and be "the best medical school in the world, for Asia".
Acknowledgements
Special thanks to A/Prof Alfred Kow Wei Chieh, A/Prof Marion Aw, A/Prof Chen Zhi Xiong and Dr Dujeepa D. Samarasekera for their guidance and constructive feedback on this article.
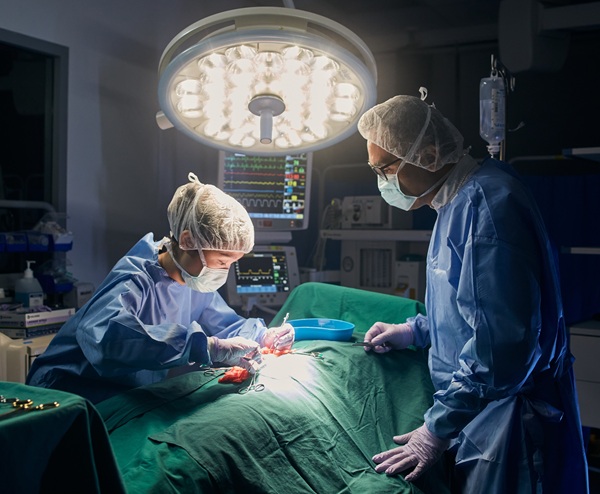
From classroom to clinical hands-on practice in a simulated OT
Asst Prof Suzanne Goh
Duke-NUS Medical School was born not out of convenience, but out of conviction. In the early 2000s, Singapore set out to develop a robust biomedical ecosystem. We thus saw a need for individuals who could contribute to scientific advancement while caring for patients – doctors who would not only practise medicine but also improve the practice of medicine. From these national ambitions emerged the vision for a graduate-entry, research-intensive medical school that would nurture clinicians with a focus on integrating scientific inquiry with clinical practice. That vision became Duke-NUS.
Our students arrive from many different countries, having completed a first degree, with some even holding Masters or PhDs. Each cohort brings a rich mix of professional and cultural backgrounds. Engineers, scientists, allied health professionals, lawyers, bankers and philosophers all learn alongside one another. Drawing strength from this diversity, we cultivate a collaborative learning environment where maturity, lived experience and interdisciplinary thinking enrich student learning.
Structure of the curriculum
Our curriculum follows a four-year structure that blends scientific foundations, clinical immersion, research training, mentorship and professional identity formation.
In Phase I, students begin with an integrated systems-based grounding in basic and applied medical sciences and learn foundational clinical and communication skills from the first day. In Phase II, students progress through core clinical clerkships, which are organised into two halves for stronger scaffolding and spiral learning, progressively deepening their clinical reasoning and patient care skills. They also complete the Research and Critical Thinking course, equipping them with essential skills for scientific inquiry and evidence-based practice.
A dedicated, immersive research period of up to nine months follows, during which students are embedded in teams led by scientists, clinicians and health system leaders addressing real problems that matter to real patients. This is not coursework, but meaningful participation in authentic scientific and clinical problem-solving: identifying needs, generating evidence, testing ideas and contributing to work that aims to improve patient care. Students gain firsthand experience of how leaders frame problems, make decisions, navigate uncertainty and integrate discovery with the realities of clinical and health system priorities, where stakes are real and the impact is immediate.
The final phase prepares students for clinical practice by exposing them to the full spectrum of patient care. In addition to their inpatient rotations, students undertake a posting in a community hospital, where they will encounter subacute, rehabilitative and transitional care. They also spend time in outpatient clinics, gaining insight into ambulatory and chronic care.
Our longitudinal integrated programme, CARE (which stands for connect, assimilate, reflect and explore), develops students across multiple threads, including ethics and professionalism, population health, procedural skills and simulation-based learning, communication, and reflective practice. Mentorship is intentionally embedded throughout the curriculum: Clinical Skills Foundation mentors are present in Phase I, CARE tutors in Phase II, research mentors in Phase III, and ambulatory care mentors in Phase IV. The four Duke-NUS colleges, led by senior clinicians serving as college masters, provide additional personal guidance, pastoral support and career advice.
Shaping identity
While the curriculum provides the structure, the heart of Duke-NUS lies in how it shapes identity. Guided by the school's mission to develop clinicians who can advance care through leadership, research and service, we recognise that becoming a doctor requires more than mastery of knowledge or technique. It requires becoming the kind of person who will serve patients, teams and society with integrity and purpose. Students engage deeply with reflection, ethics, communication, teamwork and advocacy, and these elements are woven throughout the curriculum as core educational pillars.
A particularly distinctive expression of this philosophy is the Longitudinal Ambulatory Programme, a 36-week work attachment in which students are embedded biweekly in the same outpatient clinic with the same preceptors. This model provides longitudinal mentorship and allows them to follow patients across visits, observing how conditions evolve over time, how management plans are refined and how trust is built in ambulatory care. For many, the sustained experience deepens their confidence and participation, enabling them to contribute more meaningfully to patient care and also explore a potential career path, reinforcing their growth as developing clinicians.
Threaded across the curriculum is a commitment to developing clinician-advocates. Students learn to analyse systems, recognise inequities and identify opportunities for improvement. Advocacy is expressed through clinical work, research, leadership opportunities, quality improvement and community engagement. Graduates leave with strong clinical foundations and a readiness to contribute meaningfully to the healthcare system they serve.
Today, as medicine evolves with demographic shifts, chronic disease burdens, digital transformation and AI, Duke-NUS continues to adapt. We refine how we prepare students to work responsibly with technology, navigate uncertainty, collaborate in teams and innovate thoughtfully. Our students arrive as biologists, engineers, artists and analysts, and graduate as clinicians who also contribute through research, innovation, leadership, education and service. In all these ways, we continue to pursue the Duke-NUS vision of transforming medicine and improving lives.

Student-presented research project
A/Prof Faith Chia
"If we teach today's students as we taught yesterday's, we rob them of tomorrow." – John Dewey
This quote, attributed to the great educationalist John Dewey almost a century ago, is more salient than ever in our current healthcare landscape. The rapid progress in medicine, exponential growth of technology, changing disease epidemiology and evolving patient expectations make it imperative that we not only constantly review our medical curriculum, but also equip our students with skills to allow them to be future-ready.
A reformed curriculum
LKCMedicine's foundation, built with Imperial College London, provided a strong base for curricular reform when our partnership concluded. This allowed the school to retain the best elements of the joint NTU-Imperial degree while including contemporary programme outcomes and ensuring that training is grounded in Singapore's needs, enabling graduates to be competent, adaptable and ready for future practice. The reformed curriculum also meets the requirements of MOH's National Outcomes for Medical Graduates Framework and aligns with the Healthier SG initiative and other key national healthcare shifts.
New areas of focus in the NTU Bachelor of Medicine and Surgery (MBBS) include areas of swift advancement such as digital health and AI, precision medicine, multi-morbidity and minimally disruptive medicine, preventive medicine, value-based care and health equity, to name a few. Some of these represent entirely new modules, while others strengthen or extend existing content.
The curriculum reflects Singapore's shift toward community-based care, giving students exposure to diverse community and social service settings. A longitudinal community experience developed with the Agency for Integrated Care emphasises the needs of the ageing population, nurturing doctors who understand patients' lived realities and the broader determinants of health, not just illness.
There will also be more opportunities for students to learn research skills and engage in scholarly work, culminating in a scientific symposium that allows all students to be exposed to the research journey, from planning to presentation of their work. LKCMedicine will also be introducing cadaveric dissection in Years 3 and 4 of the MBBS programme, co-led with surgeons and tying it in with surgical postings so that students will gain a greater appreciation of anatomy through the clinical lens and will be able to practise surgical skills.
Technology-enhanced learning continues to be a core feature of the NTU MBBS. Students will benefit from improved digital tools, virtual reality platforms and diverse simulation experiences. AI-powered chatbots, virtual patients and communication simulators enrich learning and provide low-stakes environments for practice. Innovative platforms also allow students to hone skills in evidence-based medicine through dynamic and interactive "sparring"opportunities.
Importantly, the NTU curriculum not only prepares students to care for patients but also has a strong focus on the learner. We are cognisant that our students will be graduating to work in a demanding healthcare system, underscoring the need to equip them for transition to practice, as well as the importance of physician well-being. Clinical teaching has more focus on realistic tasks, such as emergencies and prescribing, to better prepare students for independent practice. We identified critical transition points – especially the shift from campus to clinic and from student to practising physician – and strengthened the curriculum to better support students through these phases.
New vertical themes on professional growth and medical humanities address topics such as dealing with uncertainty, professional identity development, interprofessional teamwork, burnout and moral distress. Students will be taught practical strategies to support resilience, well-being and reflective growth – skills essential for sustaining long and meaningful medical careers. Our shift towards programmatic assessment and the Learning Progress Dashboard will allow students greater clarity regarding their learning journey, and enhance self-directed learning while being supported by their faculty and house tutors who act as coaches.
Shared vision for our learners
The journey through the curricular reform brought together over a hundred clinicians, faculty, students and alumni from LKCMedicine, partner healthcare institutions and other NTU colleges. It was heartening to see how invested the alumni and students were in building the new curriculum for their juniors, returning after clinical work on weekends to contribute, encapsulating the ethos of paying it forward. This collective process helped shape a shared vision of the ideal LKCMedicine graduate and broke down silos across themes, enabling modules to be streamlined or replaced to make space for new, relevant content.
While there is much to be excited about in the new curriculum, we also want to remember that robust clinical skills, humility, integrity and authentic compassion should be the bedrock of every physician. We want to produce strong clinicians who are rooted in values and social responsibility and support them to flourish in different areas of medicine, so that we can truly say that the LKCMedicine graduate is the doctor you and I would like to have caring for us.

LKCMedicine student Muhammad Ra'uf and Silver Generation Ambassador Doris Cheong visiting a resident as part of the community experience with the Agency for Integrated Care
